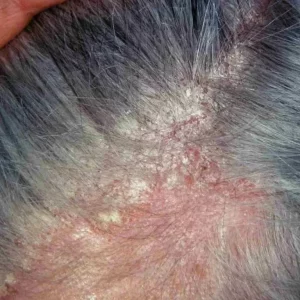
Learn How Seborrheic Dermatitis (Seb Derm) Impacts Hair Loss
Seborrheic dermatitis (seb derm) is a common chronic skin condition that affects millions of people worldwide. While it primarily manifests as red, scaly patches on the scalp and face, its impact often extends beyond the skin’s surface. One significant concern for individuals with seborrheic dermatitis is its potential connection to hair loss. Understanding how seborrheic dermatitis influences hair loss is essential for effective management and treatment. In this article, we delve into the mechanisms through which seborrheic dermatitis affects hair health, explore the relationship between inflammation and hair loss, and discuss strategies for mitigating the impact of seborrheic dermatitis on hair.
WHAT IS SEB DERM?
Seborrheic dermatitis, often abbreviated as “seb derm,” is a common chronic skin condition that primarily affects the scalp and face. It is characterized by red, scaly patches and stubborn dandruff. While the exact cause of seborrheic dermatitis is not fully understood, factors such as genetics, hormones, yeast overgrowth (specifically Malassezia), and environmental triggers are believed to play a role.
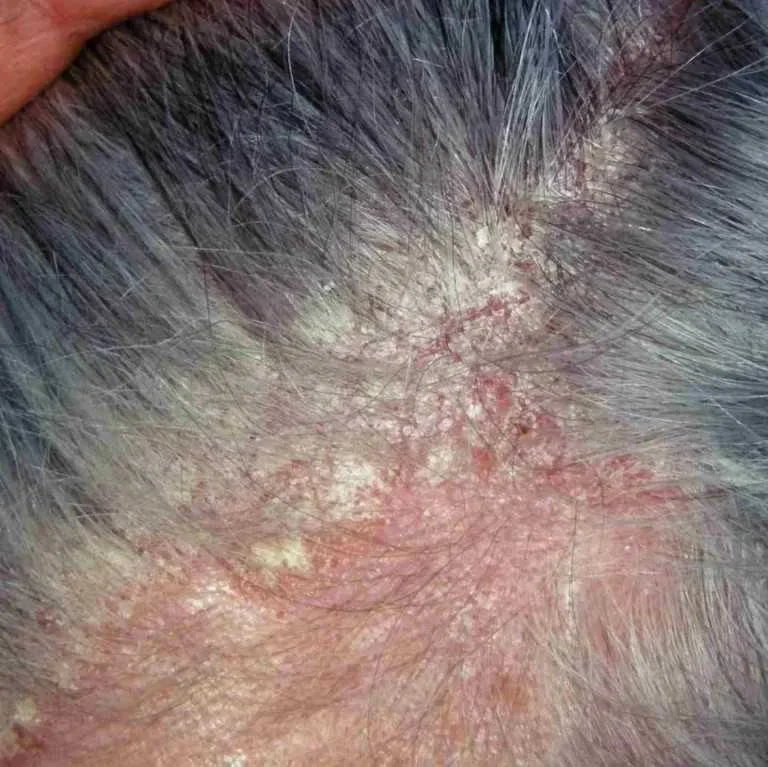
Seborrheic dermatitis can manifest differently in individuals, ranging from mild dandruff to more severe inflammation and redness. Common symptoms include flaky skin, itching, and sometimes a greasy or oily appearance.
Treatment typically involves medicated shampoos, creams, or ointments containing antifungal or anti-inflammatory ingredients to help manage symptoms and reduce flare-ups. In some cases, lifestyle changes such as reducing stress and avoiding harsh skincare products may also help alleviate symptoms. While seborrheic dermatitis can be a chronic condition, it is generally manageable with proper care and treatment.
AREAS AFFECTED BY SEB DERM
Seborrheic dermatitis, a common skin condition, exhibits a predilection for specific areas of the body characterized by an abundance of sebaceous glands. Understanding the distribution of seborrheic dermatitis lesions is crucial for accurate diagnosis and targeted treatment. Among the primary sites of involvement are the scalp, face, ears, chest, and back. Each of these areas presents distinct challenges and symptoms associated with seborrheic dermatitis, ranging from flaky scalp to red, scaly patches on facial skin. By recognizing the characteristic distribution pattern of seborrheic dermatitis, healthcare providers and individuals alike can effectively manage the condition and alleviate symptoms for improved quality of life.
- Scalp: Seborrheic dermatitis commonly affects the scalp, presenting as red, itchy, and scaly patches. This manifestation often leads to dandruff, characterized by flaking of the scalp.
- Face: Seborrheic dermatitis frequently occurs on the face, particularly in areas rich in sebaceous glands. Common sites of involvement include the eyebrows, eyelids, sides of the nose, and the area surrounding the mouth. Affected areas may exhibit redness, scaling, and greasy patches.
- Ears: Seborrheic dermatitis can affect the outer ear canal and the skin behind the ears. Symptoms may include itching, redness, and flaking of the skin.
- Chest and Back: In some cases, seborrheic dermatitis may extend to the chest and back, especially in individuals with more severe or widespread involvement. Symptoms typically resemble those observed on the scalp and face, including redness, scaling, and inflammation.
FACTORS CONTRIBUTING TO SEB DERM
Seborrheic dermatitis is a multifactorial condition influenced by a combination of genetic, environmental, and immune-related factors. Understanding the underlying mechanisms driving seborrheic dermatitis development is essential for implementing targeted therapeutic strategies. Among the key contributors are the proliferation of Malassezia yeast on the skin’s surface, genetic predisposition, hormonal fluctuations, immune system dysfunction, and environmental triggers. By elucidating these factors, healthcare providers can tailor treatment approaches to address the specific underlying causes of seborrheic dermatitis in individual patients, thereby optimizing outcomes and minimizing disease burden.
- Malassezia Yeast: Malassezia is a type of yeast that naturally inhabits the skin’s surface. In individuals prone to seborrheic dermatitis, Malassezia may proliferate excessively, leading to inflammation and skin irritation.
- Genetics: Genetic predisposition plays a significant role in seborrheic dermatitis, with a family history of the condition often observed in affected individuals. Certain genetic factors may influence skin barrier function, immune response, and sebum production, contributing to the development of seborrheic dermatitis.
- Hormonal Factors: Hormonal changes, such as those occurring during puberty, pregnancy, or menstruation, can influence sebum production and skin oiliness, potentially exacerbating seborrheic dermatitis symptoms.
- Immune System Dysfunction: Alterations in the immune system, including immune system disorders or compromised immune function, may predispose individuals to seborrheic dermatitis. Immune dysfunction can lead to an exaggerated inflammatory response to Malassezia yeast, triggering the characteristic symptoms of seborrheic dermatitis.
- Environmental and External Factors: Environmental factors such as humidity, temperature changes, and exposure to certain chemicals or irritants can exacerbate seborrheic dermatitis symptoms. Additionally, stress, fatigue, and lifestyle factors may contribute to flare-ups of the condition.
THE RELATIONSHIP BETWEEN SEB DERM AND HAIR LOSS
The relationship between seborrheic dermatitis (seb derm) and hair loss is complex, involving various mechanisms that can contribute to hair thinning and shedding. One of the primary factors contributing to hair loss in seborrheic dermatitis is inflammation. Seb derm is characterized by inflammation of the scalp, which can extend to the hair follicles. This inflammation can disrupt the normal functioning of the follicles, leading to miniaturization and weakening of the hair shaft. As a result, affected hairs may become finer and more prone to breakage, ultimately contributing to hair loss.
Inflammation associated with seborrheic dermatitis can also directly impact hair follicles by interfering with their growth cycle. Hair follicles undergo a continuous cycle of growth, rest, and shedding. However, chronic inflammation disrupts this cycle, leading to a shorter anagen (growth) phase and a prolonged telogen (resting) phase. Consequently, affected hairs may prematurely enter the shedding phase, resulting in increased hair loss.
The disruption of the hair growth cycle in seborrheic dermatitis can lead to a condition known as telogen effluvium. Telogen effluvium is characterized by excessive shedding of hair due to a disturbance in the hair growth cycle, often triggered by factors such as stress, hormonal changes, or underlying medical conditions. In seborrheic dermatitis, inflammation-induced telogen effluvium can exacerbate hair loss, further compromising hair density and thickness.
Another mechanism underlying hair loss in seborrheic dermatitis is the physical damage caused by scratching and rubbing of the affected scalp. Itching is a common symptom of seborrheic dermatitis, and persistent scratching can traumatize the scalp and hair follicles, leading to hair breakage and loss. Additionally, repeated friction and irritation from scratching can worsen inflammation and exacerbate the underlying skin condition, perpetuating a cycle of hair loss and scalp inflammation.
The relationship between seborrheic dermatitis and hair loss involves a combination of inflammation-induced follicular damage, disruption of the hair growth cycle, and physical trauma to the scalp. Understanding these mechanisms is essential for developing targeted treatment strategies aimed at preserving hair health and managing the symptoms of seborrheic dermatitis effectively. By addressing inflammation, promoting scalp hygiene, and minimizing scalp trauma, individuals with seborrheic dermatitis can mitigate the impact of the condition on hair loss and maintain healthy hair growth.
HOW SEB DERM IMPACTS HAIR LOSS
Seborrheic dermatitis (seb derm) can potentially contribute to hair loss, although the extent of its impact varies among individuals. Here’s how seborrheic dermatitis may affect hair loss:
- Inflammation of the Scalp: Seborrheic dermatitis often causes inflammation of the scalp, which can disrupt the normal hair growth cycle. Chronic inflammation may lead to damage to the hair follicles, resulting in hair thinning or even hair loss.
- Increased Shedding: Seborrheic dermatitis can lead to increased shedding of hair due to the irritation and inflammation it causes on the scalp. Excessive scratching or rubbing of the affected area can also exacerbate hair shedding.
- Disruption of the Hair Growth Cycle: Seborrheic dermatitis can disrupt the normal hair growth cycle by interfering with the follicular structure and function. This disruption may lead to shorter hair growth cycles, resulting in thinner, weaker hair over time.
- Complications from Scratching: Persistent itching associated with seborrheic dermatitis may lead to scratching of the scalp, which can further damage the hair follicles and increase the risk of hair loss. Additionally, scratching can worsen inflammation and potentially cause secondary infections, exacerbating hair loss.
- Psychological Impact: Dealing with seborrheic dermatitis and its associated symptoms, including hair loss, can be distressing for individuals. Stress and anxiety related to the condition may indirectly contribute to hair loss through mechanisms such as telogen effluvium, a type of hair loss triggered by emotional or physical stress.
While seborrheic dermatitis can be a contributing factor to hair loss, it’s essential to address the underlying condition through proper treatment and management. Using medicated shampoos, topical treatments, and following a dermatologist’s recommendations can help control seborrheic dermatitis symptoms and minimize its impact on hair health. If hair loss persists or worsens despite treatment for seborrheic dermatitis, consulting a healthcare professional for further evaluation and management is recommended.
CONSEQUENCES OF SEB DERM
Having seborrheic dermatitis (seb derm) can lead to various consequences beyond the visible skin symptoms, including increased hair shedding and damage resulting from scratching and irritation. One significant consequence experienced by individuals with seborrheic dermatitis is increased hair shedding, which can occur due to several interconnected factors. The inflammation and scaling associated with seborrheic dermatitis can disrupt the normal functioning of hair follicles, leading to weakened hair shafts that are more prone to breakage. As a result, affected individuals may notice an escalation in hair shedding, particularly during washing or brushing, exacerbating concerns about hair thinning and density.
Persistent itching, a hallmark symptom of seborrheic dermatitis, often leads to frequent scratching of the affected scalp. While scratching may provide temporary relief from itchiness, it can have detrimental effects on both the scalp and hair follicles over time. The repetitive trauma inflicted by scratching can damage the skin barrier, exacerbate inflammation, and disrupt the delicate balance of the scalp microbiome. Moreover, vigorous scratching can traumatize hair follicles, leading to hair breakage and further exacerbating hair loss. Individuals with seborrheic dermatitis may find themselves caught in a cycle of itching and scratching, inadvertently worsening the condition and its associated consequences.
In addition to hair shedding and damage, seborrheic dermatitis-related scratching and irritation can lead to secondary complications, including the development of open sores or lesions on the scalp. These lesions may increase the risk of bacterial or fungal infections, further complicating the management of seborrheic dermatitis. Moreover, the presence of visible scalp lesions can have psychosocial ramifications, affecting individuals’ self-esteem and confidence. The discomfort and embarrassment associated with scalp lesions may lead to social withdrawal and decreased quality of life, highlighting the importance of addressing the consequences of seborrheic dermatitis comprehensively.
The consequences of having seborrheic dermatitis extend beyond the primary skin symptoms, encompassing increased hair shedding, damage from scratching and irritation, and potential psychosocial impact. Recognizing these consequences underscores the importance of early intervention and effective management strategies to minimize the adverse effects of seborrheic dermatitis on both scalp health and overall well-being. By addressing inflammation, promoting scalp hygiene, and seeking appropriate medical care, individuals with seborrheic dermatitis can mitigate its consequences and achieve improved quality of life.
MANAGEMENT AND TREATMENT STRATEGIES
Managing seborrheic dermatitis-related hair loss involves a multifaceted approach that addresses both the underlying skin condition and its impact on hair health. One of the primary treatment strategies involves the use of medications and topical treatments aimed at controlling inflammation, reducing scaling, and restoring scalp health. Antifungal agents, such as ketoconazole or selenium sulfide, are commonly used in medicated shampoos to target the overgrowth of Malassezia yeast implicated in seborrheic dermatitis. These shampoos can help alleviate itching, reduce flaking, and promote scalp hygiene, thereby mitigating the inflammatory processes contributing to hair loss.
In addition to antifungal shampoos, topical corticosteroids may be prescribed to manage inflammation and redness associated with seborrheic dermatitis. These medications help suppress the immune response in the affected areas, providing relief from itching and reducing the severity of symptoms. However, long-term use of corticosteroids should be approached with caution due to the potential for side effects such as skin thinning and rebound flares upon discontinuation.
Incorporating lifestyle modifications into the management of seborrheic dermatitis-related hair loss can complement medical treatment and promote scalp health. Practicing good scalp hygiene, including regular shampooing with gentle, fragrance-free products, can help remove excess oil, debris, and scaling from the scalp, reducing the risk of flare-ups. Avoiding harsh hair care products, such as those containing sulfates or alcohol, can prevent further irritation and damage to the scalp and hair follicles.
Identifying and addressing potential triggers for seborrheic dermatitis flare-ups is essential for long-term management. Common triggers include stress, hormonal fluctuations, certain foods, and environmental factors. By adopting stress-reduction techniques, maintaining a balanced diet, and minimizing exposure to known triggers, individuals with seborrheic dermatitis can help prevent exacerbations and maintain scalp health.
In some cases, individuals with severe or refractory seborrheic dermatitis-related hair loss may benefit from additional interventions, such as phototherapy or oral medications. Phototherapy involves exposing the affected skin to ultraviolet (UV) light, which can help reduce inflammation and improve symptoms. Oral medications, such as oral antifungal agents or systemic corticosteroids, may be prescribed in cases of widespread or recalcitrant seborrheic dermatitis.
A comprehensive approach to managing seborrheic dermatitis-related hair loss includes the use of medications and topical treatments to address inflammation and scaling, along with lifestyle modifications to promote scalp hygiene and prevent flare-ups. By working closely with healthcare providers to develop personalized treatment plans, individuals with seborrheic dermatitis can effectively manage their symptoms and minimize the impact of the condition on hair health and overall well-being.
CONCLUSION
Seborrheic dermatitis presents a multifaceted challenge for individuals, extending beyond its characteristic skin symptoms to potentially impact hair health and quality of life. The interplay of inflammation, disruption of the hair growth cycle, and physical trauma from scratching underscores the complexity of the relationship between seborrheic dermatitis and hair loss. However, by understanding the mechanisms underlying hair loss in seborrheic dermatitis and implementing targeted management strategies, individuals can mitigate its impact and achieve improved outcomes. From medicated shampoos and topical treatments to lifestyle modifications and personalized interventions, there exists a range of options for effectively managing seborrheic dermatitis-related hair loss. Moreover, early intervention and consistent adherence to treatment regimens are crucial for minimizing the progression of hair loss and promoting scalp health. By addressing both the skin condition and its consequences on hair health comprehensively, individuals with seborrheic dermatitis can take proactive steps towards restoring confidence, comfort, and overall well-being.
SHOP FOR HAIR LOSS TREATMENTS